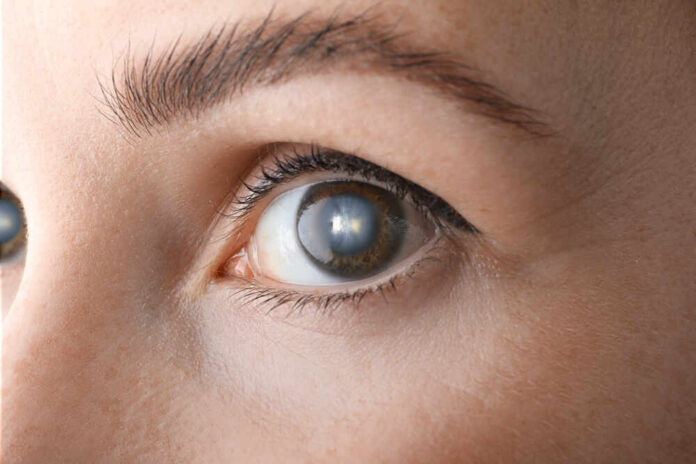
Your eyes can lose critical vision quietly after 40, and the scariest part is you often won’t feel a thing until damage sticks.
Quick Take
- Schedule comprehensive eye exams because glaucoma and retinal disease can advance without obvious symptoms.
- Block ultraviolet light year-round; consistent UV exposure connects to cataract risk, and good lenses must cover UVA and UVB.
- Eat for your retinas: leafy greens, omega-3s, and key antioxidants tie back to major research on slowing AMD progression.
- Use screen rules and dry-eye habits to keep daily strain from becoming chronic irritation and blurry focus.
The post-40 eye shift: why “fine” isn’t a medical measurement
Presbyopia makes near vision tougher for almost everyone, but it’s the headline that distracts from the quiet risks. Cataracts can build over years, macular degeneration can steal fine detail, and glaucoma can damage the optic nerve long before you notice peripheral loss. Adults over 40 sit in the zone where prevention finally beats “wait and see,” because early detection still offers choices instead of regrets.
Eye care after 40 works best when it runs like home maintenance: routine inspection, small fixes early, and fewer emergencies later. Conservative, common-sense health habits shine here because they reduce downstream dependence—less crisis care, fewer expensive procedures, and more independence. The goal is not perfection; it’s stacking practical advantages. That starts with one unglamorous move most people delay until something goes wrong.
Comprehensive eye exams: the highest-return appointment you’ll make
Book a comprehensive eye exam on a schedule your provider recommends, and tighten that schedule if you have diabetes, high blood pressure, a family history of glaucoma, or other risk factors. Clinics now use advanced imaging such as OCT in many settings, helping catch subtle changes earlier. That matters because glaucoma often progresses without pain, and early retinal changes don’t announce themselves with dramatic symptoms.
Ask direct questions and get direct answers: What is my eye pressure? How do my optic nerves look? Did you examine my retina after dilation, and what should I watch for at home? People over 40 sometimes accept “you’re fine” as a complete report; it’s not. A real baseline lets you track change, and in eye health, change is the whole story.
UV protection: sunglasses are medical gear, not a fashion accessory
Wear sunglasses that block 100% of UVA and UVB, and treat coverage like a safety feature. Wraparound styles reduce light sneaking in from the sides, and a brimmed hat adds another layer during peak sun hours. Epidemiology links a meaningful share of cataracts to UV exposure, so daily protection behaves like long-term insurance: cheap upfront, expensive to skip, and painfully obvious only after years.
Demand the label and ignore the hype. Dark lenses without proper UV protection can backfire by dilating pupils while still letting damaging rays through. Keep a pair in the car, by the door, and in your travel bag so “I forgot” stops being the reason you absorb the most sun. Consistency beats intensity; steady protection wins the decade.
Eat to defend the retina: the AREDS lesson most people oversimplify
Nutrition advice turns into noise until you anchor it to outcomes. The Age-Related Eye Disease Study showed a measurable reduction in the risk of progression for certain AMD patients using a specific nutrient combination. That finding didn’t make vegetables optional; it made diet strategy concrete. Build meals around leafy greens, colorful produce, and omega-3 sources, then treat supplements as targeted tools for the right people.
Use food first because it stacks benefits across the body: blood vessels, inflammation, and metabolic health all influence ocular outcomes. Zinc and antioxidant discussions can get gimmicky; don’t let marketing replace medical guidance. If you’re high-risk for AMD or already diagnosed, ask your eye doctor whether an AREDS-style formula fits your case and what tradeoffs matter for you.
Lifestyle levers that protect sight: no-nonsense habits that compound
Exercise supports circulation, and your eyes depend on steady blood flow. Sleep repairs tissues, and chronic sleep debt often shows up as irritation, dryness, and fluctuating focus. Hydration helps tear film stability, which becomes more fragile with age. Smoking remains one of the most self-defeating choices for long-term eye health, stacking oxidative stress on top of aging biology for no practical upside.
Alcohol moderation also matters because dehydration and disrupted sleep can amplify dry-eye symptoms and visual fatigue. These are not trendy “biohacks”; they’re the same conservative principles that keep everything running longer: avoid obvious harm, maintain the system, and don’t trade tomorrow’s function for today’s convenience. Eye care is simply where those principles get shockingly visible.
Screens and the 20-20-20 rule: how modern life quietly drains comfort
Digital eye strain doesn’t usually destroy vision, but it can make daily life miserable and can mask other issues. Use the 20-20-20 rule: every 20 minutes, look at something 20 feet away for 20 seconds. Blink more than feels natural, because screen focus reduces blinking and dries the ocular surface. Adjust lighting and font size so your eyes stop brute-forcing clarity.
Blue-light conversations often turn political or profit-driven; keep it practical. Reduce glare, avoid screen use right before bed if it wrecks sleep, and treat persistent headaches or blurry episodes as a reason to get checked—not as a reason to buy another gadget. Comfort is a performance metric. When your eyes feel better, your patience, productivity, and driving confidence usually follow.
Control the chronic conditions that sabotage vision in the background
Diabetes and hypertension can damage small blood vessels, including those feeding the retina and optic nerve. That connection turns routine primary care into eye care. Keep A1C and blood pressure targets in range, take medications as prescribed, and don’t improvise with “natural” substitutes that haven’t earned the evidence. People who value self-reliance should treat chronic disease control as the most direct path to staying independent longer.
Watch for the open loop most people miss: you can do everything else and still lose ground if chronic conditions run wild. Pair your eye-exam schedule with your primary-care schedule so nobody owns only half the picture. When you align habits, screenings, and medical management, you build a simple system that protects sight year after year.
Sources:
Eye Care Checklist for Adults Over 40
Eye Care After 40: What Changes to Expect
5 Eye Conditions That Become More Common After 40
Adult Vision: 41 to 60 Years of Age
Common Age-Related Eye Problems














