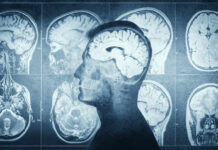
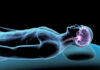
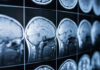
A massive review of decades of trials reveals zero high-quality proof that cannabis eases anxiety, depression, or PTSD—the top reasons millions turn to it.
Story Snapshot
- Largest RCT analysis ever: 50+ trials, 2,500 patients over 45 years show no solid evidence for core mental health uses.
- Researchers call data scarcity “embarrassing,” with zero depression studies and weak results elsewhere.
- Federal Schedule I rules block better research, despite 38+ state legalizations and booming $30B market.
- Experts warn of risks like psychosis in youth; calls grow for real trials amid hype.
Landmark Review Exposes Evidence Void
Researchers at the Matilda Centre, University of Sydney, analyzed over 50 randomized controlled trials from 1981 to 2026, covering nearly 2,500 patients. They found no high-quality evidence cannabis treats anxiety, depression, or PTSD symptoms. Lead author Jack Wilson stresses routine use lacks justification without data. This meta-analysis excluded weaker observational studies for rigor.
The review identified limited low-quality evidence for insomnia, autism, and Tourette’s syndrome benefits. Depression had zero qualifying RCTs. Anxiety and PTSD trials showed inconsistent, poor results. Publication in The Lancet Psychiatry on March 2026 marks the strictest scrutiny yet. NPR covered it March 17, 2026, highlighting public use outpacing science.
Historical Barriers Stifle Gold-Standard Research
U.S. federal law classified cannabis Schedule I in 1970, blocking funding and access for rigorous RCTs despite centuries of medicinal claims. California’s 1996 legalization sparked modern surge, with mental health topping self-reported uses alongside pain. By 2026, 38 states allow medical cannabis, yet trials lag. A prior JAMA Internal Medicine review echoed inefficacy and risks for vulnerable groups.
2010s state expansions boosted access but not quality data. Early 2026 JAMA paper warned adolescents and psychosis-prone face harms. Lancet findings quantify the gap: public assumes relief without proof. Potential Trump-era rescheduling signals change, easing research hurdles.
Stakeholders Clash on Science vs. Access
Jack Wilson pushes evidence-based policy against routine prescribing. Ryan Vandrey of Johns Hopkins calls data collection embarrassing, noting some patients improve while others worsen. Ziva Cooper at UCLA highlights CBD promise for anxiety but urges broader evidence. Joel Gelernter from Yale argues cannabis causes more PTSD than it cures, demanding RCTs first.
Academics influence via journals; DEA and FDA gatekeep trials. Medical industry meets patient demand despite gaps, creating prescriber tensions with illicit markets. Patient advocates prioritize access; regulators weigh reform.
🧬 Huge study finds no evidence cannabis helps anxiety, depression, or PTSD
Cannabis for mental health? Think again
Read more → https://t.co/VUJ42BdozO#Science #Health pic.twitter.com/a6unLicr39
— SkimNews (@SkimNews_) March 20, 2026
Impacts Ripple Through Patients and Markets
Short-term, clinicians pause unproven scripts for top conditions, protecting youth from psychosis links seen in precedents. Long-term, pressure builds for funded RCTs reshaping guidelines. Anxiety, depression, PTSD patients question self-treatment; $30B cannabis sector eyes pivots to pain or insomnia.
Socially, “natural remedy” myths crack under facts. Vulnerable communities gain warnings; mental health prioritizes therapies with backing.
Sources:
Sparse evidence for cannabis to treat mental health conditions highlights research gap
2018 PMC commentary on psychosis risks
Yale study on cannabis use disorder and psychiatric risks