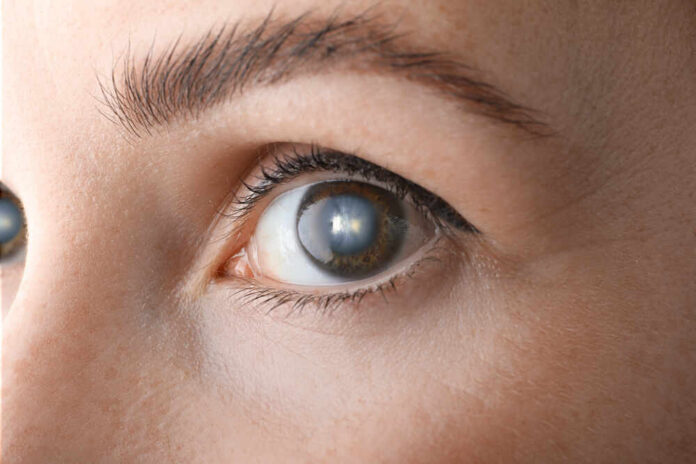
A newly identified protein may hold the key to preventing diabetic blindness before it even starts, upending decades of late-stage treatment strategies and offering millions a chance to keep their sight.
Story Snapshot
- University College London scientists pinpointed LRG1 protein as the earliest trigger of diabetic retinopathy, acting before the well-known VEGF pathway kicks in
- Blocking LRG1 in diabetic mice prevented retinal capillary damage and preserved vision, demonstrating true prevention rather than damage control
- A clinical-grade LRG1-targeting antibody already exists and is in final preclinical testing before human trials
- Nearly one-third of adults with diabetes show retinopathy signs, making this discovery relevant to hundreds of millions worldwide
The Protein That Squeezes Blood Vessels Shut
Researchers at the UCL Institute of Ophthalmology discovered that LRG1 drives pathological constriction of pericytes, the cells that wrap around tiny retinal blood vessels like a support scaffold. When diabetes triggers LRG1 production, these pericytes essentially squeeze capillaries shut, choking off oxygen supply to the retina and setting the stage for a cascade of damage that ultimately leads to vision loss. This mechanism operates upstream of VEGF, the growth factor that has dominated diabetic eye disease treatment for years, explaining why anti-VEGF drugs only work after significant damage has already occurred.
Prevention Before Damage, Not Rescue After
The team, led by Dr. Giulia De Rossi, demonstrated in diabetic mouse models that both genetic deletion and pharmacologic blockade of LRG1 prevented early vascular injury and preserved retinal function. This represents a fundamental shift from the current paradigm, which relies on laser photocoagulation and anti-VEGF injections to manage late-stage disease after structural damage and vision loss have begun. De Rossi frames the discovery bluntly: diabetic eye disease starts earlier than previously thought, and LRG1 is the key culprit in this early damage, offering a way to protect vision before serious damage occurs.
A Drug Already Waiting in the Wings
What sets this discovery apart from typical academic breakthroughs is therapeutic readiness. The UCL team has already developed what they describe as a tried and tested LRG1-targeting antibody, now in final laboratory studies before moving to first-in-human clinical trials. This speed from discovery to potential therapy stems from prior work on LRG1 in angiogenesis and vascular remodeling in other tissues, allowing researchers to leverage existing antibody platforms. The work was funded by Diabetes UK, Moorfields Eye Charity, and Wellcome, organizations that prioritize translating basic research into clinical benefit rather than letting findings languish in journals.
Filling the Gap in a Half-Billion-Person Problem
Diabetic retinopathy remains a leading cause of blindness in working-age adults across developed countries, progressing from early non-proliferative stages with microaneurysms and hemorrhages to proliferative disease with dangerous new blood vessel growth. Current treatments address symptoms after the fact, and a significant subset of patients do not respond adequately to anti-VEGF therapy. LRG1-targeted therapy could serve dual purposes: as a preventive treatment for high-risk individuals with early microvascular changes, and as an alternative for late-stage patients who have exhausted anti-VEGF options. The economic implications are substantial, potentially reducing surgical interventions, injection burdens, and disability costs associated with blindness.
The Biomarker Race Alongside the Drug Race
Parallel research is identifying stage-specific protein signatures in the aqueous humor of diabetic retinopathy patients, with proteins like S100A7 rising early and APOB and TF spiking in severe stages. These proteomic profiles offer companion diagnostic potential, helping clinicians identify precisely which patients would benefit most from LRG1-targeted intervention. Advanced imaging modalities that detect retinal vascular leakage before visual acuity drops are also maturing, creating the infrastructure for a true early-detection, early-intervention model. This convergence of therapeutic target, biomarker science, and functional imaging represents a rare alignment in translational medicine.
From Lab Bench to Eye Clinic
The study appeared in Science Translational Medicine in October 2025, with UCL and Diabetes UK announcing findings that reframe diabetic retinopathy pathogenesis around LRG1-driven pericyte constriction and hypoxia. Diabetes UK’s Dr. Faye Riley emphasized that retinopathy is one of the most feared complications of diabetes, and identifying the root cause of early damage offers a new treatment path with immense promise for protecting sight globally. The therapeutic timeline is aggressive: final preclinical work is underway, with human trials targeted for the near future. If early-phase safety and efficacy data hold up, LRG1 inhibitors could enter clinical guidelines within a handful of years, marking the first true preventive biologic for diabetic eye disease.
Sources:
Scientists discover early trigger of diabetic eye disease, paving the way for new treatments – UCL
Our scientists discover early trigger of diabetic eye disease – Diabetes UK
Proteomics reveals protein shifts in diabetic eye disease – ASBMB Today
Scientists Uncover the ‘Root Cause’ Triggering Early Diabetic Blindness – SciTechDaily
Everyday diabetes medicine may prevent common causes of blindness – Medical Xpress
Uncovering how occludin protein maintains blood-brain and blood-retinal barriers – Michigan Medicine
Research: Protein deletion could treat age- and diabetes-induced eye diseases – Eyewire News